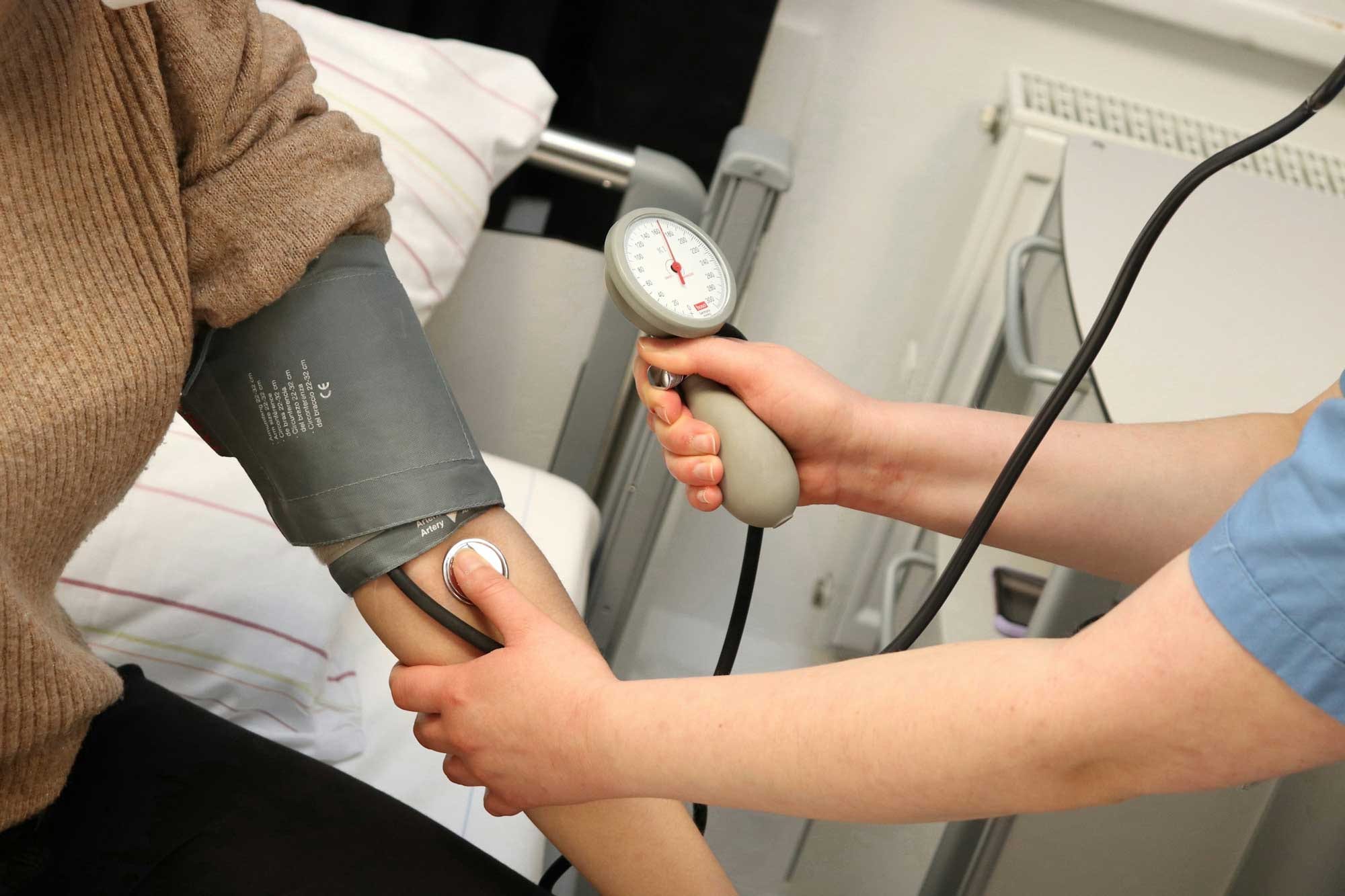
Diabetes blood pressure management is one of the most important – yet often overlooked – aspects of long-term diabetes care. When diabetes and hypertension occur together, the risk of serious health problems rises dramatically. From heart attacks and strokes to kidney failure and vision loss, uncontrolled blood pressure can accelerate diabetes complications at an alarming rate.
If you are living with type 2 diabetes and blood pressure concerns, understanding how these conditions interact is essential. The good news is that with proper blood pressure control in diabetes, lifestyle changes for diabetics, and evidence-based medical care, you can significantly reduce your diabetes and heart disease risk.
In this comprehensive guide, we explore the science behind diabetes and hypertension, the risks of poor control, recommended targets, actionable lifestyle strategies, and medical treatments that protect your heart, kidneys, brain, and blood vessels.
Understanding the Connection Between Diabetes and Hypertension
Diabetes and hypertension frequently occur together. Research shows that people with type 2 diabetes are significantly more likely to develop high blood pressure compared to those without diabetes. This is not a coincidence – both conditions share underlying metabolic and vascular mechanisms.
How High Blood Sugar Damages Blood Vessels
Persistently elevated blood glucose levels damage the inner lining of blood vessels, a process known as endothelial dysfunction. Over time, blood vessels become stiffer, narrower, and less able to relax. This increases resistance to blood flow, raising blood pressure.
In addition, insulin resistance – a hallmark of type 2 diabetes – causes the body to retain more sodium through the kidneys. Sodium retention increases fluid volume, which further elevates blood pressure.
Obesity, chronic inflammation, and hormonal imbalances also contribute to the powerful link between diabetes and hypertension.